
Telehealth Disease Management can Modulate a Coming Wave of Delayed Non-COVID Illness Treatment
Featured in MCOL Blog’s Payers and Providers, June 2020
By: Peter Anderson, AristaMD advisor
The COVID-19 pandemic may not end in America for another year or more. While this prospect is daunting, a major secondary national health challenge could also be imminent. This “second surge” may not just be the follow-on COVID-19 wave many fear, although that could also occur. Instead, experts worry that a potentially massive influx of non-COVID-19 related acute and chronic health cases is looming as stay-at-home orders start being relaxed and patients begin going back to their providers.
This pent-up demand for care has been described as a “crisis within a crisis.”
The U.S. healthcare system has been so focused on the coronavirus in recent months that it appears that treatment of other health needs is being delayed or ignored. Because of this, patients may overwhelm the system when medical facilities reopen and/or care can no longer be postponed.
In addition to healthy patients forgoing standard care, evidence shows that acutely and chronically ill patients have not received the treatment they need since the pandemic began, whether a vital drug prescription or a potentially life-saving medical or surgical procedure. Stakeholders and leaders across the healthcare spectrum are recognizing this upcoming surge amongst the current and upcoming challenges the virus poses.
“I am worried about hidden illness due to foregone care and how this might contribute to a ‘second wave’ related to this pandemic.”
David Chokshi, M.D.
Internist, Bellevue Hospital in New York
Documenting Care Delays
The parameters of the approaching challenge are already taking shape. A recent, large-scale national patient survey showed that 53 percent of respondents were worried about catching the novel coronavirus if they visited medical facilities for non-COVID-19 health issues.
According to William P. Jaquis, MD, president of the American College of Emergency Medicine, emergency department visits in parts of the U.S. are, in fact, down by as much as 50%.
Experts now estimate that nearly one in three Americans have delayed needed healthcare during the pandemic.
“I would estimate we have had at least 15 deaths not related to COVID … people staying at home and hoping they get better instead of seeking treatment – and they’re dying.”
Eric Snyder, M.D.
Medical Director, Providence Cedars-Sinai Tarzana Medical Center in California
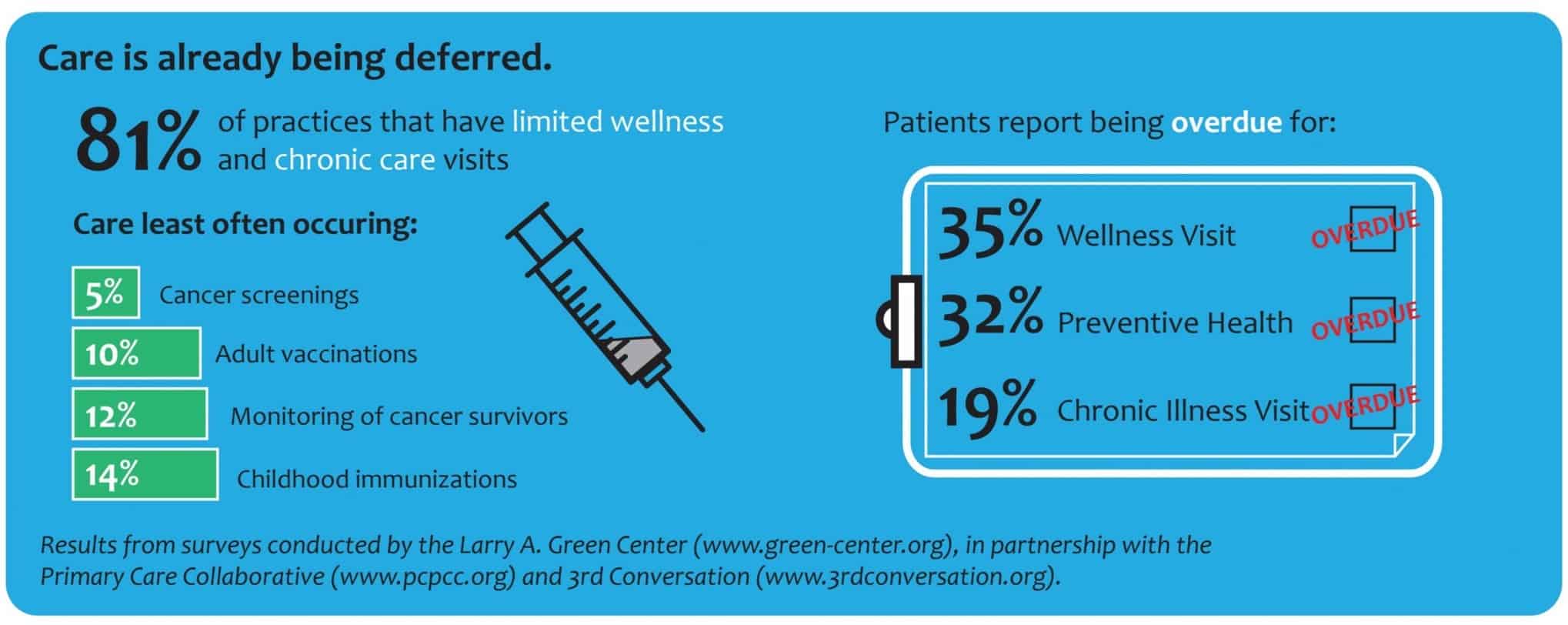
Source: www.pcpp.org, www.green-center.org, www.3rdconversation.org
Reasons for avoiding or delaying care include:
- Individuals’ fear of virus exposure
- State, county, or municipal stay-at-home orders
- Inability to afford care due to job loss during the pandemic
- Temporary closure of medical offices to try to control COVID-19 spread
- Inability to access open facilities because of the volume of COVID-19 cases
Preventive care, such as cancer screenings, has been particularly hard hit, with appointments for cervix, colon and breast cancer screenings down between 86% and 94% compared to typical volumes. And older Americans, who are at high risk for the coronavirus, are avoiding medical care in significant numbers.
A recent survey of more than 1,000 elderly adults found that 39% had canceled or delayed medical treatment.
Chronic Diseases are a Particular Concern
A study done following the SARS virus outbreak of 2002-2004 showed that hospitalizations for diabetes plummeted during that crisis, then rose dramatically afterwards. The damage patients incur by delaying treatment for chronic diseases like diabetes, heart disease and cancer can be irreversible, and experts fear that the experience post-SARS will be repeated on a far larger scale during and after the COVID-19 pandemic.
Doctors know that chronically ill patients will clamor to get the care they need once the virus is no longer perceived as a threat—and that the “second surge” may be starting even now, when COVID-19’s danger is still very real.
Leveraging Tools to Manage the Surge
Awareness that a wave of non-COVID cases is both inevitable and impending means that now is the time to find tools and resources to decelerate the deluge. Experts say that if healthcare organizations take the right steps now, the impact can be lessened—at least to some degree.
The good news is that, in part because of the pandemic, physicians and healthcare organizations are recognizing the value of telehealth disease management and have implemented various telemedicine modalities at an expedited pace compared to previously slow-moving adoption. Remote forms of healthcare, including online and phone visits, are being used with much greater frequency, successfully providing quality care for both COVID and non-COVID-related concerns.
It’s also become clear that, when primary care providers (PCPs) and specialists work together through telehealth disease management platforms like electronic consultation, or eConsults, PCPs’ ability to deliver the full scope of patient care is enhanced.
During the past few months, when our healthcare system has been stretched to its limits, eConsults have:
- Helped PCPs easily and quickly access specialty care expertise
- Reduced the need for patients to visit specialists’ waiting rooms and hospital emergency departments
- Limited unnecessary exposure to COVID-19 for both patients and providers
Using eConsult technology, medication adjustments can be recommended remotely by a specialist, and the patient’s PCP can then carry out that adjustment, sometimes also on a remote basis. This is especially important for at-risk patient populations such as older adults, people with chronic conditions, and immunocompromised patients.
Healthcare Success Post-COVID-19 Requires Patient Triage
eConsults ensure patients are appropriately triaged to the most appropriate care setting as we approach the “second surge.”
For healthcare organizations, eConsults are a tool to process referral queues and triage members into one of the following four categories:
- Patients that specialists should see remotely via telemedicine
- Patients that can be treated or have additional work-ups or diagnostics completed within primary care
- Patients that need face-to-face specialty appointments immediately
- Patients that need face-to-face specialty appointments but less urgently
Effective triage will benefit all healthcare stakeholders:
- Health systems: by managing care in the most appropriate setting and optimizing revenue streams
- Payors: by ensuring patients can access care within the most appropriate setting
- Providers: by reducing backlog burden and providing a tool to provide more total patient care
- Patients: by improving access to timely care, whether it be virtual, within primary care, or specialist office if needed (with decreased appointment wait times)
Maximizing Patient Health with Telehealth Disease Management and eConsults
At this point, no one knows if or when our healthcare system will fully return to pre-pandemic norms. What we do know is that telehealth disease management tools and, specifically, eConsults, are already increasing patient health and safety. The benefits of eConsult platforms include:
- Providing both acute and chronic disease patients with fast and safe access to specialty care, even while stay-at-home regulations are in place
- Ensuring that patients maintain continuity for essential specialty care
- Keeping low-acuity patients from becoming higher-acuity because they delay needed care
- Extending capacity at specialist offices when they re-open, avoiding a potential patient logjam
Simply put, delays in medical care are bad for our health–the health of our population and the organizations that provide care. That’s one reason that, in the era of COVID-19, medical professionals and health care organizations are adopting telehealth disease management tools at an extraordinary rate.
Among those tools, eConsult platforms excel at providing on-demand specialty care. These platforms can not only prevent the negative health impact of care delays, they can also help reduce the size of the upcoming second surge as COVID-19 restrictions are removed.
